decision support system (DSS)
What is a decision support system (DSS)?
A decision support system (DSS) is a computer program application used to improve a company's decision-making capabilities. It analyzes large amounts of data and presents an organization with the best possible options available.
Decision support systems bring together data and knowledge from different areas and sources to provide users with information beyond the usual reports and summaries. This is intended to help people make informed decisions.
Typical information a decision support application might gather and present include the following:
- comparative sales figures between one week and the next;
- projected revenue figures based on new product sales assumptions; and
- the consequences of different decisions.
A decision support system is an informational application as opposed to an operational application. Informational applications provide users with relevant information based on a variety of data sources to support better-informed decision-making. Operational applications, by contrast, record the details of business transactions, including the data required for the decision-support needs of a business.
Decision support system components
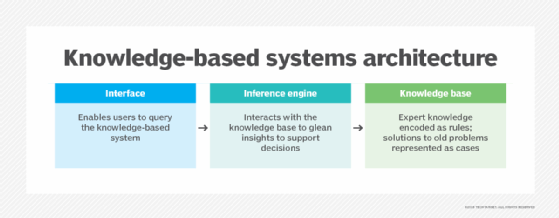
A typical DSS consists of three different parts: knowledge database, software and user interface.
Knowledge base. A knowledge base is an integral part of a decision support system database, containing information from both internal and external sources. It is a library of information related to particular subjects and is the part of a DSS that stores information used by the system's reasoning engine to determine a course of action.
Learn about knowledge base uses in customer service and call centers.
Software system. The software system is composed of model management systems. A model is a simulation of a real-world system with the goal of understanding how the system works and how it can be improved. Organizations use models to predict how outcomes will change with different adjustments to the system.
For example, models can be helpful for understanding systems that are too complicated, too expensive or too dangerous to fully explore in real life. That's the idea behind computer simulations used for scientific research, engineering tests, weather forecasting and many other applications.
Models can also be used to represent and explore systems that don't yet exist, like a proposed new technology, a planned factory or a business's supply chain. Businesses also use models to predict the outcomes of different changes to a system -- such as policies, risks and regulations -- to help make business decisions.
User interface. The user interface enables easy system navigation. The primary goal of the decision support system's user interface is to make it easy for the user to manipulate the data that is stored on it. Businesses can use the interface to evaluate the effectiveness of DSS transactions for the end users. DSS interfaces include simple windows, complex menu-driven interfaces and command-line interfaces.
Intelligent decision support system (IDSS)
Users can also bake artificial intelligence (AI) into decision support systems. Called intelligent decision support systems (IDSS), the AI mines and processes large amounts of data to get insights and make recommendations for better decision-making. It does this by analyzing multiple sources of data and identifying patterns, trends and associations to emulate human decision-making capabilities.
Designed to act similar to a human consultant, an IDSS gathers and analyzes data to support decision-makers by identifying and troubleshooting issues, and providing and evaluating possible solutions. The AI component of the DSS emulates human capabilities as closely as possible, while more efficiently processing and analyzing information as a computer system.
The IDSS may include advanced capabilities such as a knowledge base, machine learning, data mining and a user interface. Examples of IDSS implementations include flexible or smart manufacturing systems, intelligent marketing decision support systems and medical diagnostic systems.
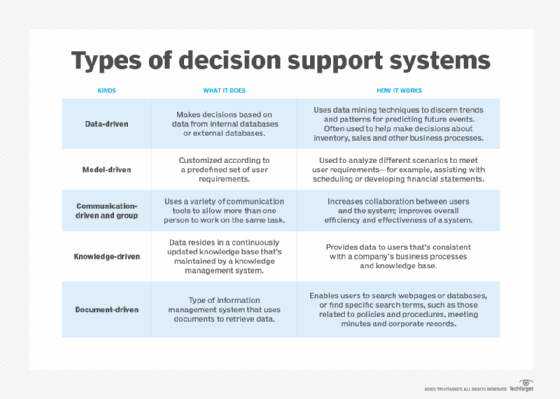
Types of decision support systems
Decision support systems can be broken down into categories, each based on their primary sources of information.
Data-driven DSS
A data-driven DSS is a computer program that makes decisions based on data from internal databases or external databases. Typically, a data-driven DSS uses data mining techniques to discern trends and patterns, enabling it to predict future events. Businesses often use data-driven DSSes to help make decisions about inventory, sales and other business processes. Some are used to help make decisions in the public sector, such as predicting the likelihood of future criminal behavior.
Model-driven DSS
Built on an underlying decision model, model-driven decision support systems are customized according to a predefined set of user requirements to help analyze different scenarios that meet these requirements. For example, a model-driven DSS may assist with scheduling or developing financial statements.
Communication-driven and group DSS
A communication-driven and group decision support system uses a variety of communication tools -- such as email, instant messaging or voice chat -- to allow more than one person to work on the same task. The goal behind this type of DSS is to increase collaboration between the users and the system and to improve the overall efficiency and effectiveness of the system.
Knowledge-driven DSS
In this type of decision support system, the data that drives the system resides in a knowledge base that is continuously updated and maintained by a knowledge management system. A knowledge-driven DSS provides information to users that is consistent with a company's business processes and knowledge.
Document-driven DSS
A document-driven DSS is a type of information management system that uses documents to retrieve data. Document-driven DSSes enable users to search webpages or databases, or find specific search terms. Examples of documents accessed by a document-driven DSS include policies and procedures, meeting minutes and corporate records.
Learn more about the differences between knowledge management and information management here.
Decision support system examples
Organizations use decision support systems in several different contexts, including the following:
- GPS routing. GPS route planning is an example of a typical DSS. It compares different routes, taking into account factors such as distance, driving time and cost. The GPS navigating system also enables users to choose alternative routes, displaying them on a map and providing step-by-step instructions.
- ERP dashboards. ERP (enterprise resource planning) dashboards can use a decision support system to visualize changes in production and business processes, monitor current business performance against set goals and identify areas for improvement. ERP dashboards let business owners see a snapshot of their company's most important numbers and metrics.
- Clinical decision support system. A clinical decision support system (CDSS) is a software program that uses advanced decision-making algorithms to help physicians make the best medical decisions. Healthcare professionals often use these to interpret patient records and test results, and to calculate the best treatment plan. CDSS in healthcare can help providers identify abnormalities during specific tests, as well as monitor patients after certain procedures to determine if they are having any adverse reactions.







