Health IT (health information technology)
Health IT (health information technology) is the area of IT involving the design, development, creation, use and maintenance of information systems for the healthcare industry. Automated and interoperable healthcare information systems will continue to improve medical care and public health, lower costs, increase efficiency, reduce errors and improve patient satisfaction, while also optimizing reimbursement for ambulatory and inpatient healthcare providers.
Today, the importance of health IT results from the combination of evolving technology and changing government policies that influence the quality of patient care. Modern health IT received a boost when President George W. Bush introduced incentives for hospitals to adopt electronic health record (EHR) systems, and that march has continued with Presidents Barack Obama and Donald Trump, showing that health IT enjoys general bipartisan support.
Types of health information technology
The EHR is the central component of the health IT infrastructure. An EHR, or electronic medical record (EMR), is a person's official, digital health record and is shared among multiple healthcare providers and agencies. Other key elements of the health IT infrastructure are the personal health record (PHR), which is a person's self-maintained health record, and the health information exchange (HIE), a health data clearinghouse or a group of healthcare organizations that enter into an interoperability pact and agree to share data between their various health IT systems. Thanks to smartphones and other mobile devices, in the coming years, PHRs will grow in popularity as consumers become more comfortable with their digital health information. Thus, PHRs will need to integrate further with EHR technology.
As a result of the mountain of patient information that healthcare organizations now sit on, data analytics has taken a greater role in day-to-day operations. The ability to aggregate patient information, analyze it and then base treatments on the results fits in well with population health management (PHM) and value-based healthcare. Artificial intelligence will take analytics to a higher level, although, as of 2018, AI is not relied upon for diagnoses. Analytics also raises the question of who owns the data: the patient, the healthcare organization or the vendor that produced the analytics software? Trends in healthcare point to patients ultimately becoming the owners.
There are other important health IT technologies beyond EHRs. Picture archiving and communication systems (PACS) and vendor-neutral archives (VNAs) are two widely used types of health IT that help healthcare professionals store and manage patients' medical images. In the past, radiology departments have been the primary repositories of medical images, but PACS and VNAs are integrating radiology into the main hospital workflow. And other specialties, such as cardiology and neurology, have also become large-scale producers of clinical images. In some instances, VNAs have been installed as a way to merge imaging data stored in separate departments' image banks in a multifacility healthcare system.
Improvements in health technology include patient portals, which are not new but are enjoying a second wind at hospitals and physician practices thanks to more consumer-friendly designs. In earlier days, a patient portal may have been a clunky site that enabled patients to view upcoming visits and perhaps see raw lab test results. By comparison, modern portals provide more context to a patient's care. The portals let patients securely communicate with their physicians, pay bills, check services against what an insurance plan allows, download full medical records, order prescriptions and possibly interact with a chatbot for other services.
Portals may also integrate with telemedicine systems, which enable secure video conversations between patients and providers. As the ease and convenience of video conferencing improves, telemedicine will be an important piece of the healthcare experience for patients who may need to speak to a physician or nurse face-to-face but do not necessarily need an in-office visit.
More recent innovations in health IT technology include the greater use of the application program interface (API) to improve interoperability, the ability to access and interact with health data via mobile devices and further exploration of blockchain as a way to better access and secure medical records.
Regulations and oversight
Implementations of EHR systems have increased dramatically in the past few years since the inception of the Health Information Technology for Economic and Clinical Health (HITECH) Act in 2009, which introduced EHR incentive programs and the related meaningful use program. Physicians and hospitals that proved their use of government-certified EHR systems met meaningful use criteria -- created and overseen by the Centers for Medicare & Medicaid Services (CMS) and the Office of the National Coordinator for Health IT (ONC) -- were eligible to receive incentive payments totaling tens of billions of dollars across the U.S. healthcare industry.
Meaningful use is changing to a new value-based reimbursement system under a law passed by Congress in 2015 called MACRA, the Medicare Access and CHIP (Children's Health Insurance Program) Reauthorization Act. Meanwhile, the 21st Century Cures Act of 2016 poured $6 billion into medical research using leading-edge technology and science.
Also, healthcare organizations and their business associates, such as third-party billing companies, that handle protected health information (PHI) are subject to the Health Insurance Portability and Accountability Act (HIPAA), created and enforced by the U.S. Department of Health and Human Services (HHS). The law mandates that patients have full access to their PHI and protects the privacy of their information by limiting access to it by other parties. A healthcare provider that experiences a breach of PHI can be fined by the HHS Office for Civil Rights (OCR).
Security and privacy
HIPAA's security and privacy rules have long guided healthcare organizations to provide patients access to their medical records, while also safeguarding that information.
Such goals have taken on greater urgency given that data breaches and malware attacks have scourged the healthcare industry since 2010. Nearly 5.6 million patients had their records breached in 2017, and although the amount of patient data breaches dropped that year, malware and ransomware attacks on healthcare sites increased, according to a 2018 report from Protenus, a health IT privacy and security firm.
In response, traditional health IT systems now often integrate with data security and cybersecurity technology. Worker education is also part of the solution, as human errors can lead to data breaches.
Changes to the workforce
As in many industries, IT managers and chief information officers (CIOs) in healthcare organizations have risen in authority as technology becomes more prevalent.
The growing position of informatician, or informaticist, ties directly to the expansion of health IT. Under health informatics and its variants, professionals manage and study health IT and patient data together. Informaticians may have an IT background or a clinical background, but in both cases, these people combine science, medical treatments and IT. For example, a clinical informaticist could be someone with a background as a bedside nurse who transitions to an IT-based role.
Also, there is a subset of practicing physicians and nurses who have also become experts in health IT and patient data matters. Although these clinicians remain firmly embedded in patient care, they are able to more easily converse with IT about their needs and the technology options available.
In a broader sense, health IT has affected every clinician who has trained on an EHR or telemedicine systems, and working with this technology has become a core job skill.
Benefits of health information technology
While some critics say EHRs have led to clinicians spending more time entering data than conversing with patients and produced cumbersome federal regulations, there is broad consensus on the benefits of health IT. These advantages include:
- the ability to use data analytics and big data to effectively manage population health management programs and reduce the incidence of expensive chronic health conditions;
- the use of cognitive computing and analytics to perform precision medicine (PM) tailored to individual patients;
- the ability to share health data among academic researchers to develop new medical therapies and drugs; and
- the rights of patients to obtain and use their own health data and collaborate in their own care with clinicians.
Other health IT challenges
Some major challenges persist in health IT. Chief among them are obstacles to interoperability, including a lack of commonly agreed-on health data interchange standards, although the health IT standard-developing organization HL7 International (Health Level Seven) has developed and promulgated several popular standards -- most recently, FHIR (Fast Health Interoperability Resources).
Also, federal officials and patient advocates have identified as a pervasive problem the alleged practice of information blocking by some vendors and providers in an attempt to stymie the ability to share health data in their systems. Health regulators have made it increasingly clear that they will not tolerate information blocking.
Major vendors
For a long time, the health IT world was led by vendors that specialized in electronic health records and other niche healthcare technology.
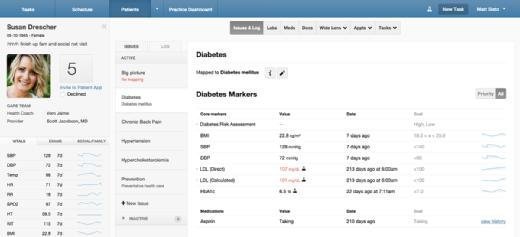
Epic Systems and Cerner Corporation have battled for the No. 1 EHR seller spot, with Allscripts and Meditech behind the big two. AthenaHealth Inc. has gained steam based on its cloud-based EHR systems.
Change Healthcare -- the health IT spinoff of pharmaceutical distributor McKesson Corporation -- is looking at cutting-edge health IT, including blockchain. Medical imaging systems are sold by well-known vendors, including General Electric (GE) and Fujifilm.
All of these sellers are now looking over their shoulders as huge, non-health IT tech companies, such as Apple, Google and Amazon, make inroads into the healthcare industry.
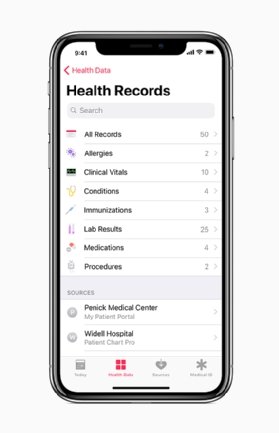
For example, in 2018, Apple began to successfully test technology that enabled its Apple Health app to integrate patient PHRs with hospital EHRs, and Cerner and Epic were also involved in those tests. Meanwhile, Amazon, JPMorgan Chase and Berkshire Hathaway planned to create an independent healthcare company for their workers, using health IT to aid the project.
Also, Google and Fitbit announced a partnership around Google's new cloud healthcare API, which is based on FHIR.






